To know more about Orthopedic Doctor-Click Here
To Know more about concessions offered by AFI on Joint Replacement & Arthroscopy in Delhi-NCR- Click Here
What is Arthroscopy?
Arthroscopy is a surgical procedure by which the internal structure of a joint is examined for diagnosis and/or treatment using a tube-like viewing instrument called an arthroscope also called pinhole surgery. When performed in the outpatient setting, patients can usually return home on the same day otherwise 1-2 day admission is sufficient for all the procedures done by this technique.
The technique of arthroscopy involves inserting the arthroscope, a small tube that contains optical fibers and lenses, through tiny incisions in the skin into the joint to be examined. The arthroscope is connected to a video camera and the interior of the joint is seen on a television monitor. The size of the arthroscope varies with the size of the joint being examined. For example, the knee is examined with an arthroscope that is approximately 5 millimeters in diameter. Smaller arthroscopes also available.
If procedures are performed in addition to examining the joint with the arthroscope, this is called arthroscopic surgery. Usually causes less tissue trauma, results in less pain, and promotes quicker recovery.
The main indications are:
• To identify the problems inside the joint e.g. torn cartilage, loose bodies, intra- articular fractures, tear of ligaments etc.
• Confirmation of the diagnosis
• Synovial Biospy for say TB knee
• Lavage: just washing the joint with normal saline produces relief of pain for a remarkable period. specially in mild to moderate types of osteo-arthritis of the knee joint.
• Synovial lesions like villonodular synoritis
• Articular cartilage lesions.
• Meniscal tears
Mostly after clinical examination & X-Ray; MRI findings are very helpful in assessment of pathology. But it is important to mention that MRI findings can have a percentage of error.
What is done in preparation for arthroscopy?
Arthroscopy is essentially a very low blood loss procedure and has very few complications. The underlying health of the patient is considered when determining who is a candidate for arthroscopy. Most importantly, the patient should be able tolerate the anesthesia that is used during the procedure. A person's heart, kidney, liver, and lung function should be adequate. If there are existing problems such as heart failure or emphysema, these should be optimized as possible prior to surgery. Patients who are on anticoagulants (blood thinners) should have these medications carefully adjusted prior to surgery. Other medical problems should also be controlled prior to surgery, such as diabetes and high blood pressure. Preoperative evaluation of a patient's health will generally include a physical examination, blood tests, and a urinalysis. Patients who have a history of heart or lung problems and generally anyone over the age of 50 will usually be asked to obtain an electrocardiogram (EKG) and a chest X-ray. Any signs of ongoing infection in the body usually postpones arthroscopy, unless it is being done for possible infection of the joint in question.
How is arthroscopy performed?
The patient will check into the facility where the procedure is being performed and an intravenous line (IV) established in order to administer fluids and medication. The type of anesthesia used varies depending on the joint being examined and the medical health of the patient. Arthroscopy can be performed under a general anesthetic, a spinal or epidural anesthetic, a regional block (where only the extremity being examined is numbed), or even a local anesthetic. If a general anesthetic is not used, the patient is often sedated.After adequate anesthesia is achieved, the procedure can begin. An incision is made on the side of the joint to be examined and the arthroscope is inserted into the incision. Other instruments are sometimes placed in another incision to help maneuver certain structures into the view of the arthroscope. In arthroscopic surgery, additional instruments for surgical repairs are inserted into the joint through additional small incisions in the joint. These instruments can be used to cut, remove, and suture (sew) damaged tissues. Once the procedure is completed, the arthroscope in removed and the incisions are sutured closed. A sterile dressing is placed over the incision and a brace or ACE wrap may be placed around the joint.
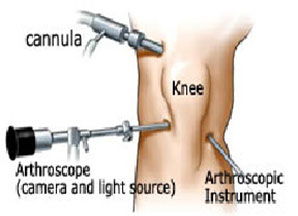
Knee arthroscopy
Knee arthroscopy is surgery that uses a tiny camera to look inside your knee. Small cuts are made to insert the camera and small surgical tools into your knee for the procedure.
Description
Three different types of pain relief (anesthesia) may be used for knee arthroscopy surgery:
• Local anesthesia. Your knee may be numbed with pain medicine. You may also be given medicines that relax you. You will stay awake.
• Spinal anesthesia. This is also called regional anesthesia. The pain medicine is injected into a space in your spine. You will be awake but will not be able to feel anything below your waist.
• General anesthesia. You will be asleep and pain-free.
• Femoral nerve block. This is another type of regional anesthesia. The pain medicine is injected around the nerve in your groin. You will be asleep during the operation. This type of anesthesia will block out pain so that you need less general anesthesia.
A cuff-like device may be put around your thigh to help control bleeding during the procedure.
The surgeon will make two or three small cuts around your knee. Salt water (saline) will be pumped into your knee to inflate the knee.
A narrow tube with a tiny camera on the end will be inserted through one of the cuts. The camera is attached to a video monitor that lets the surgeon see inside the knee.
The surgeon may put other small surgery tools inside your knee through the other cuts. The surgeon will then fix or remove the problem in your knee.
At the end of your surgery, the saline will be drained from your knee. The surgeon will close your cuts with sutures (stitches) and cover them with a dressing. Many surgeons take pictures of the procedure from the video monitor, You may be able to view these pictures after the operation so that you can see what was done.
Why the Procedure is Performed
Arthroscopy may be recommended for these knee problems:
• Torn meniscus. Meniscus is cartilage that cushions the space between the bones in the knee. Surgery is done to repair or remove it.
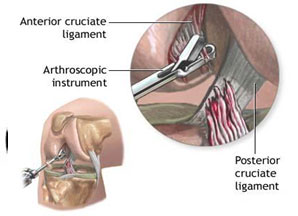
• Torn or damaged anterior cruciate ligament (ACL) or posterior cruciate ligament (PCL)
• Swollen (inflamed) or damaged lining of the joint. This lining is called the synovium.
• Kneecap (patella) that is out of position (misalignment).
• Removal of Baker's cyst. This is a swelling behind the knee that is filled with fluid. Sometimes the problem occurs when there is swelling and pain (inflammation) from other causes, like arthritis.
• Repair of defect in cartilage
• Some fractures of the bones of the knee
Risks
The risks for anesthesia and surgery are:
Additional risks for this surgery include:
• Bleeding into the knee joint
• Infection in the knee joint
• Knee stiffness
Recovery / Outcome
Usually for small procedures like meniscal tears recovery is fest & 1 to 2 weeks are enough for ligament reconstructions ACL/PCL partial weight bearing walk 3 weeks & full weight bearing 6 weeks outcomes usually gratifying.
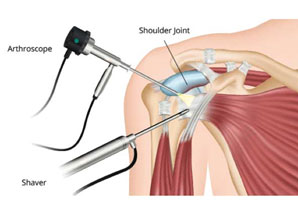
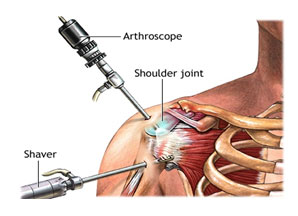
Shoulder arthroscopy
Shoulder arthroscopy is surgery that uses a tiny camera called an arthroscope to examine or repair the tissues inside or around your shoulder joint. The arthroscope is inserted through a small cut (incision) in your skin.
Description
The rotator cuff is a group of muscles and their tendons that form a cuff over the shoulder joint. These muscles and tendons hold the arm in the shoulder joint and help the shoulder move in different directions. The tendons in the rotator cuff can tear when they are overused or injured.
You will likely receive general anesthesia before this surgery. This means you will be asleep and unable to feel pain. Or, you may have regional anesthesia. Your arm and shoulder area will be numbed so that you do not feel any pain. If you receive regional anesthesia, you will also be given medicine to make you very sleepy during the operation.
During the procedure, the surgeon:
• Inserts the arthroscope into your shoulder through a small incision. The scope is connected to a video monitor in the operating room.
• Inspects all the tissues of your shoulder joint and the area above the joint. These tissues include the cartilage, bones, tendons, and ligaments.
• Repairs any damaged tissues. To do this, your surgeon makes 1 to 3 more small incisions and inserts other instruments through them. A tear in a muscle, tendon, or cartilage is fixed. Any damaged tissue is removed.
Your surgeon may do one or more of these procedures during your operation:
Rotator cuff repair:
• The edges of the tendon are brought together. The tendon is attached to the bone with sutures.
• Small rivets (called suture anchors) are often used to help attach the tendon to the bone.
• The anchors can be made of metal or plastic. They do not need to be removed after surgery.
Surgery for impingement syndrome:
• Damaged or inflamed tissue is cleaned out in the area above the shoulder joint.
• A ligament called the coracoacromial ligament may be cut.
• The underside of a bone called the acromion may be shaved. A bony growth (spur) on the underside of the acromion often causes impingement syndrome. The spur can cause inflammation and pain in your shoulder.
Surgery for shoulder instability:
• If you have a torn labrum, the surgeon will repair it. The labrum is the cartilage that lines the rim of the shoulder joint.
• Ligaments that attach to this area will also be repaired.
• The Bankart lesion is a tear on the labrum in the lower part of the shoulder joint.
• A SLAP lesion involves the labrum and the ligament on the top part of the shoulder joint.
At the end of the surgery, the incisions will be closed with stitches and covered with a dressing (bandage). Most surgeons take pictures from the video monitor during the procedure to show you what they found and the repairs that were made.
Your surgeon may need to do mini open or open surgery if there is a lot of damage. Open surgery means you will have a large incision so that the surgeon can get directly to your bones and tissues.
Risks/ complications : Usually are in Arthroscopy
• Bleeding, blood clots, infection
• Shoulder stiffness
• Failure of the surgery to relieve symptoms
• The repair fails to heal
• Weakness of the shoulder
• Injury to a blood vessel or nerve
Preparation
Preparation of surgery is generally like another surgery.
After the Procedure
Follow any discharge and self-care instructions you are given.
Recovery can take 1 to 3 months. You will probably have to wear a sling for the first week. If you had a lot of repair done, you may have to wear the sling longer.
You may take medicine to control your pain.
When you can return to work or play sports will depend on what your surgery involved. It can range from 1 week to several months.
Physical therapy may help you regain motion and strength in your shoulder. The length of therapy will depend on what was done during your surgery.
Outlook (Prognosis)
Arthroscopy often results in less pain and stiffness, fewer complications, a shorter (if any) hospital stay, and faster recovery than open surgery.
If you had a repair, your body needs time to heal, even after arthroscopic surgery, just as you would need time to recover from open surgery. Because of this, your recovery time may still be long.
Surgery to fix a cartilage tear is usually done to make the shoulder more stable. Many people recover fully, and their shoulder stays stable. But some people may still have shoulder instability after arthroscopic repair.
Using arthroscopy for rotator cuff repairs or tendinitis usually relieves the pain, but you may not regain all of your strength.
Hip Arthroscopy
Hip arthroscopy is not as commonly used procedure as knee & shoulder is initially used for the diagnosis of unexplained hip pain, but is now widely used in the treatment of conditions both in and outside the hip joint. The most common indication currently is for the treatment of femoroacetabular impingement (FAI) and its associated pathologies. Hip conditions that may be treated arthroscopically also includes labral tears, loose / foreign body removal, hip washout (for infection) or biopsy, chondral (cartilage) lesions, osteochondritis dissecans, ligamentum teres injuries (and reconstruction), Iliopsoas tendinopathy (or ‘snapping psoas’), trochanteric pain syndrome, snapping iliotibial band, osteoarthritis (controversial), sciatic nerve compression (piriformis syndrome), ischiofemoral impingement and direct assessment of hip replacement.

